|
What dangerous effects result from pulmonary edema?ģ-4.How does the body attempt to protect the lungs from edema?ĥ. What is treatment for cardiogenic pulmonary edema? 1-2. Elevated = cardiogenic, normal or low = non-cardiogenicġ6. Use a pulmonary wedge (balloon in pulmonary arteries) and measure pressure. First patient sign is often orthopnea (shortness of breath when supine) can be relieved when sitting upright.ġ5. Sepsis- when chemicals released into blood stream to fight infection, trigger inflammatory response. Non-cardiogenic = due to direct injury to alveolar epithelium after primary injury to capillary endothelium.ħ. Cardiogenic = increase in left atrial pressure, resulting in an increase in venous pressure resulting in an increase in capillary pressure. What are the lymphatic obstruction/removal causes that can cause lymphedema? What are the circulating agents that can increase capillary permeability? These cause increase fluid and possibly protein filtration resulting in edema 1-5. What are the causes of decreased vascular oncotic pressure (πc)? What is the primary cause of an increased interstitial osmotic pressure leading to edema? Lymphedema also causes an increase in πIF 1. These act as osmotic agents in fluid accumulation and non-pitting edema. Primary cause is thyroid dysfunction (elevated mucopolysaccharides in the interstitum). What are the causes to an increase in capillary hydrostatic pressure leading to edema? Elevated blood volume (Na+ retention) (heart failure) 1-3. Increase in venous pressure (venous obstruction or heart failure)ģ. Marked increase in blood flow (vasodilation)Ģ. What are the two primary causes to peripheral edema? Why does lymphedema produce the edema mentioned in the previous question? What type of edema does lymphedema produce?Ħ. How can you distinguish between pitting edema and non-pitting edema?ĥ. What types of edema respond well to diuretic therapy?Ĥ. What is the most common type of edema?Ģ-3. 
πIF increases, thus fluid will continue to remain in this area even after palpated. 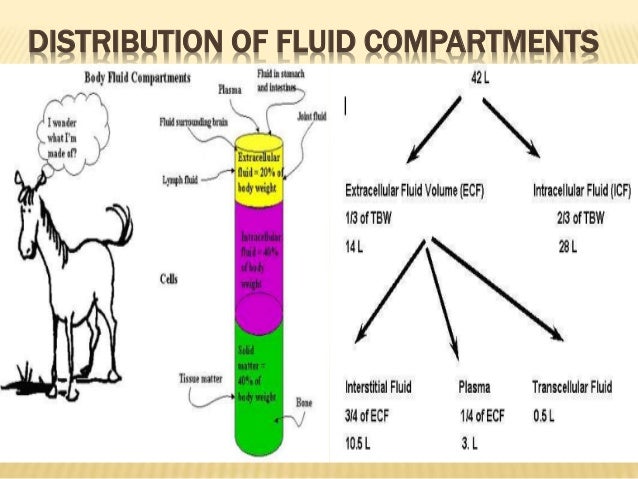
This is not the case in Non-pitting edema.Ħ. Pressing affected area with a finger or thumb results in a visual indentation of the skin that persists after the digit is removed in Pitting edema. Non-pitting edema = does not respond well to diuretic therapy (diuretic therapy does not take care of the problem of the osmolarity, rather it is a temporary fix)Ĥ. Pitting edema = responds well to diuretic therapy What are the function of lymphatics as they relate to fluid movement? What is the relationship between lymphatic flow and interstitial pressure?Ģ-3. Maintain low interstitial volume and low protein content by removing proteins and fluids from the interstitum. They are proportional/directly related.Ģ-3. What protein is the largest contributor to πc?Ģ.What is the formula for fluid movement according to the Starling Equation? Albumin synthesized in the liver, is the most abundant plasma protein and thus the biggest contributor to oncotic pressure of plasmaĤ. Hydrostatic pressure (blood pressure) in the capillary is directly related to which 3 factors? 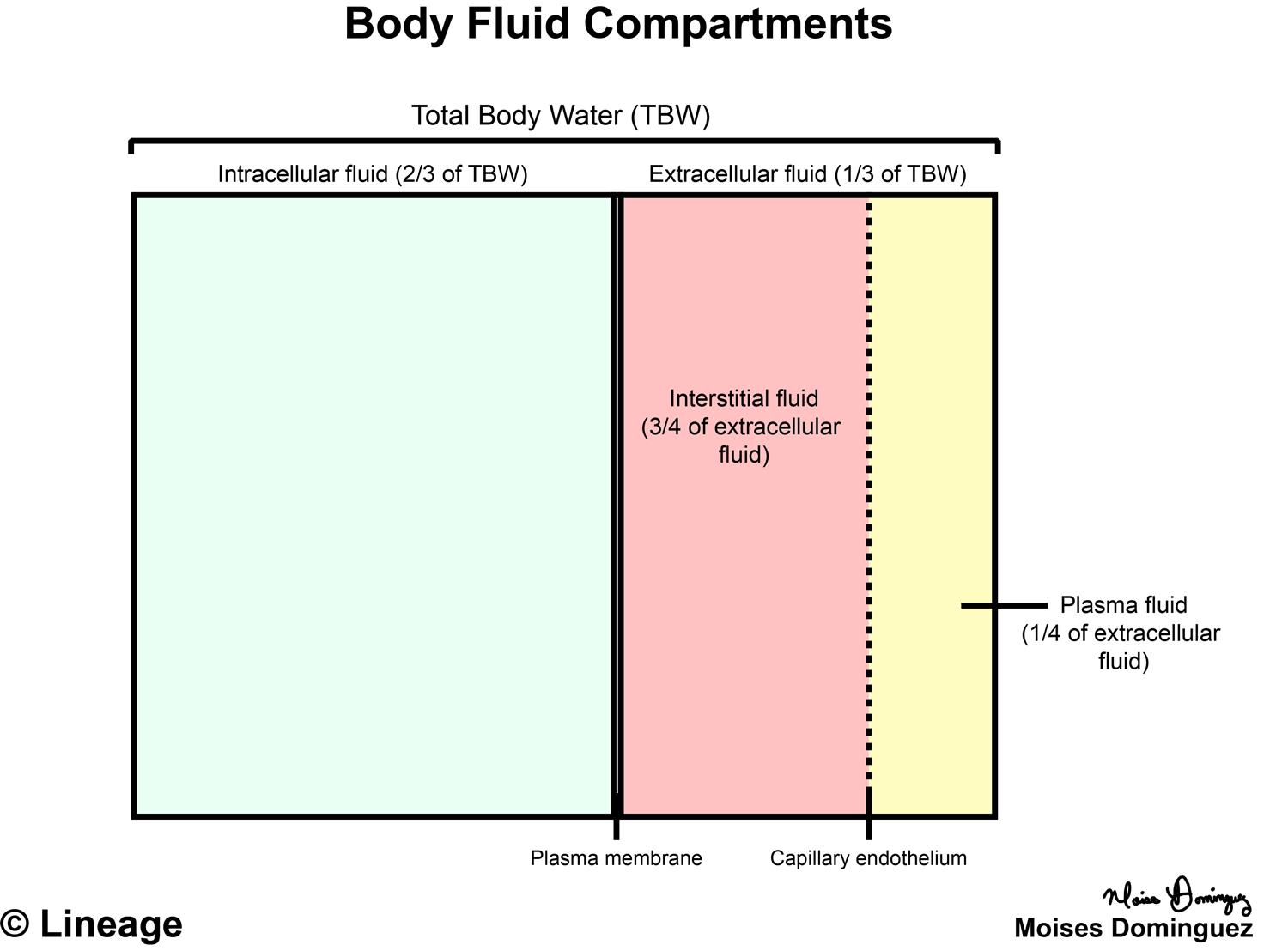
Blood flow (regulated at the arteriole)ģ. What exception to the previous two forces is there that can make this force a significant factor? What are forces rarely make a impact on the exchange of a fluid?ħ. What are the forces for fluid absorption?ĥ-6. What are the forces for fluid filtration?ģ-4. PIF- It becomes a significant factor if edema is present, or it can affect glomerular filtration in the kidney (pressure in Bowman's space is analogous to interstitial pressure) 1-2. πc = oncotic (osmotic) force in the interstitumħ. PIF = hydrostatic pressure in the interstitumĤ. πIF = oncotic (osmotic) force in the interstitumģ. Pc = Hydrostatic pressure (blood pressure) in the capillaryĢ. What are the primary 3 regulators of Renin? What is the primary function of Renin?Ģ-4. Na+ delivery to the macula densa (ascending portion where distal convoluted tubule begins) an increase inhibits// a decrease stimulates Reninġ. Sympathetic stimulation to the kidney (direct effect via Beta-1 receptors)Ĥ. Perfusion pressure of kidney (inversely related) an increase inhibits// a decrease stimulatesģ. catalyzes conversion of angiotensinogen to angiotensin I which in turn is converted to Ang II by Angiotensin converting enzyme (ACE).Ģ.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
